Definition of Torn Meniscus
Last Updated 11/08/20 by Cory Calendine, MD, Orthopedic Surgeon
A torn meniscus is a tear in the cartilage of the knee. The knee is made up of the femur (thigh bone), the tibia (leg bone), and the patella (knee cap). Between the femur and the tibia are two pads that function to improve the fit between the femur and the tibia and act as shock absorbers within the knee joint. Each of these pads is called a meniscus: 1) Medial Meniscus (inside of knee), 2) Lateral Meniscus (outside of knee).
Each meniscus is made of C-shaped fibrocartilage and contains collagen fibers which help maintain its shape and integrity. A torn meniscus is one of the most common knee injuries, and can occur from trauma or from wear-and-tear degeneration. Any activity that involves forcefully twisting or rotating the knee, especially when applying full weight onto the joint, can lead to a torn meniscus. Conservative treatment — such as rest, ice and medication — is sometimes enough to relieve the pain of a torn meniscus and give the injury time to heal on its own. However, only about 1/5 of knee meniscus tissue has an active blood supply (outer margin). Meniscus tissue that lacks blood supply is unlikely to heal on its own if it is torn and often requires surgical repair.
Meniscus Tear Symptoms
If you've torn your meniscus, you might have the following signs and symptoms in your knee:
- A popping sensation
- Swelling or stiffness
- Pain, usually worse during twisting or squatting motions.
- Difficulty straightening your knee fully
- catching or locking of the knee
- Feeling of your knee giving way
Following the initial injury, the pain and swelling from a meniscus tear may improve. However, athletic activities and certain movements, such as going up and down stairs or getting in and out of cars, may reproduce pain in a knee with a torn meniscus. The pain can interfere with correct muscle coordination during activity and lead to a dangerous "giving way" sensation of the knee joint.
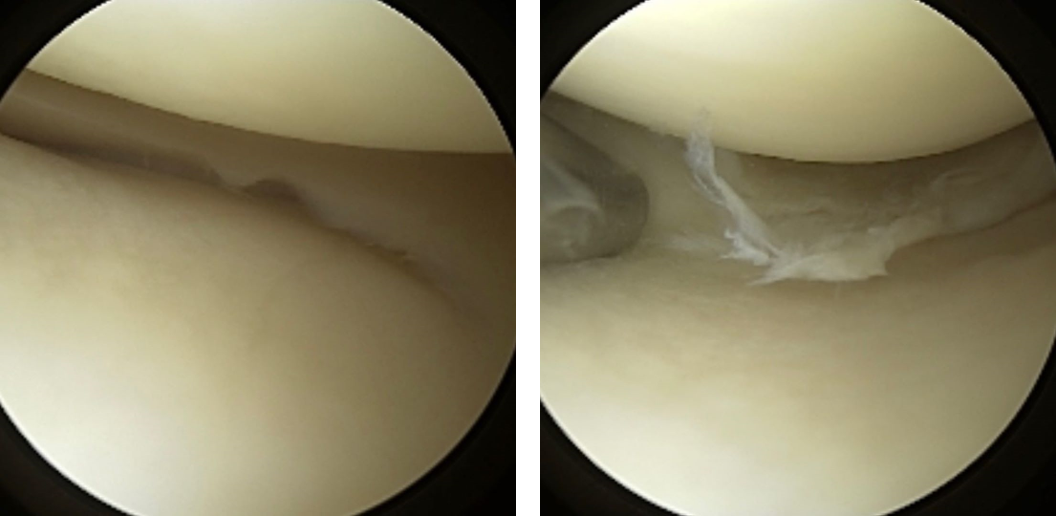
The pain, swelling, catching and locking of a meniscus injury can be relieved by surgically removing or repairing the torn piece of meniscus. In the case of meniscus tears associated with degenerative changes and osteoarthritis, the treatment recommendations can differ – osteoarthritis in the knee is frequently associated with small degenerative meniscal tears and vice versa. The acute symptoms from a new degenerative meniscal tear (pain and swelling) may resolve over a few months time without immediate surgical intervention. However, mechanical symptoms such as catching or locking of the knee joint are less likely to resolve without surgery.
Knee Meniscus Tear: Diagnosis and Treatment
A torn meniscus can often be diagnosed via physical exam. The doctor will look for swelling, tenderness along the joint line, loss of motion, and pain with certain movements of the knee joint. An MRI can be used to confirm the diagnosis of a torn meniscus.
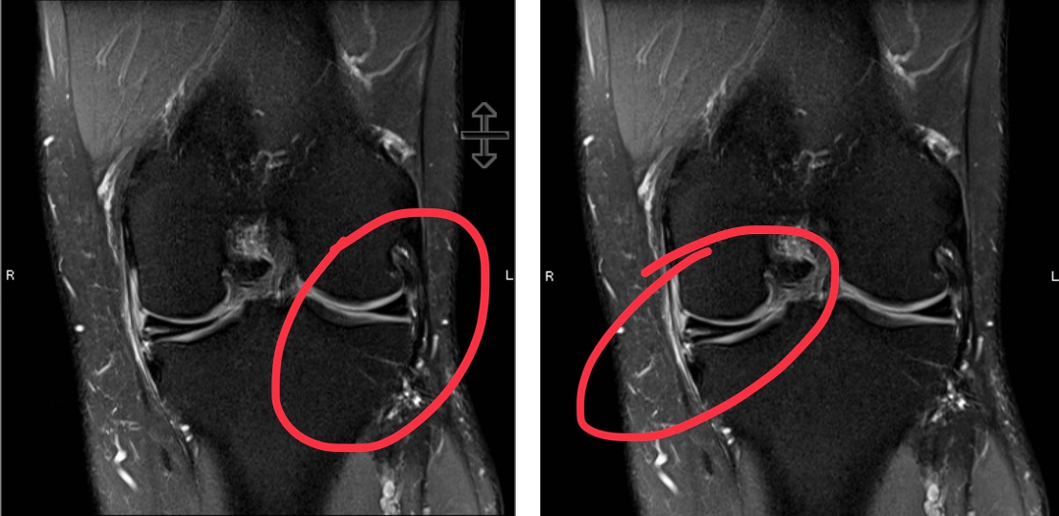
Arthroscopic surgery to remove or repair torn menisci is the definitive treatment for meniscal tears. A meniscus tear that does not cause the knee to catch or lock is less likely to cause damage to the rest of the knee, and pain and swelling symptoms can be treated symptomatically without surgery. The pain can be treated initially with over the counter pain medications such as acetaminophen or ibuprofen. Pivoting/squatting movements should initially be minimized as patients are encouraged to maintain and optimize leg muscle strength. Quadriceps muscle strengthening exercises can help prevent some of the secondary effects of a torn meniscus such as knee cap pain or the sense of buckling. If the swelling and pain does not resolve with conservative therapy (within 6 weeks), surgical intervention may be required.
Knee Meniscus Surgery
Surgery is the definitive treatment for torn meniscus. The surgery is done arthroscopically and will include either removal or repair of the torn part of meniscus. Repair can be completed if the tear lies near the zone of the meniscus with a sufficient blood supply.
In the case of a degenerative meniscal tear associated with osteoarthritis, although surgically treating the torn meniscus and trimming away damaged articular cartilage caused by the arthritis may eliminate the mechanical catching or locking of the knee joint, the non-mechanical symptoms of osteoarthritis (stiffness, achiness, weather-related pain) may persist. Therefore, in the setting of a degenerative meniscal tear with osteoarthritis, the surgeon also needs to discuss treatment alternatives for joint arthritis such as knee injections and partial or total knee replacement.
RELATED:
Summary of Torn Knee Meniscus
- Meniscal tears occur from trauma or degeneration or a combination of the two.
- Meniscal tears can produce knee pain, swelling, catching, and locking.
- Most meniscal tears do not heal because they are in an anatomic area that has no blood supply.
- The definitive treatment for meniscal tears is arthroscopic surgery.




.jpg)



