X-rays, CT Scans and MRIs
by Cory Calendine, MD, Orthopaedic Surgeon, Hip and Knee Specialist
Diagnostic imaging techniques can help delineate musculoskeletal injury and disease. The most commonly used techniques include xrays, computed tomography (CT) scans, and magnetic resonance imaging (MRI).
These imaging tools allow surgeons to "see" inside the body and get a "picture" of the bones, organs, muscles, tendons, nerves, and cartilage.
Xrays
Due to cost and availability, xrays (radiographs) are the most commonly ordered diagnostic imaging modality. Even if a more complex test is required for final diagnosis, xray is often used as a first-line screen.
Xrays use low doses of radiation to image dense objects including bones, calcifications, some tumors, and other dense matter. More dense objects appear white or lighter on xray films because they absorb the radiation. Less dense soft tissues structures allow the radiation pass-through, therefore appear darker on xray films.
Computed tomography (CT)
CT is an imaging technique that combines xray images from various angles with computer technology that produces more detailed, cross-sectional images of the body. CT scans allow surgeons to visualize 3D size, shape, and position of structures that are deeper within the body and joints. CT scans are more expensive and take more time than regular xray imaging.
Magnetic Resonance Imaging (MRI)
Magnetic resonance imaging (MRI) uses radio waves to produce detailed cross-sectional images of the body. Unlike xrays and CT scans, MRI does not require the use of radiation. MRI machines use magnetic fields and computer processing to take high-resolution pictures of bones and soft tissues.
Due to the ability to generate more detailed images – especially of soft tissues - MRI can be used to better evaluate ligaments, tendons and cartilage surfaces. MRI scans typically take longer and are more expensive than xrays and CT scans.
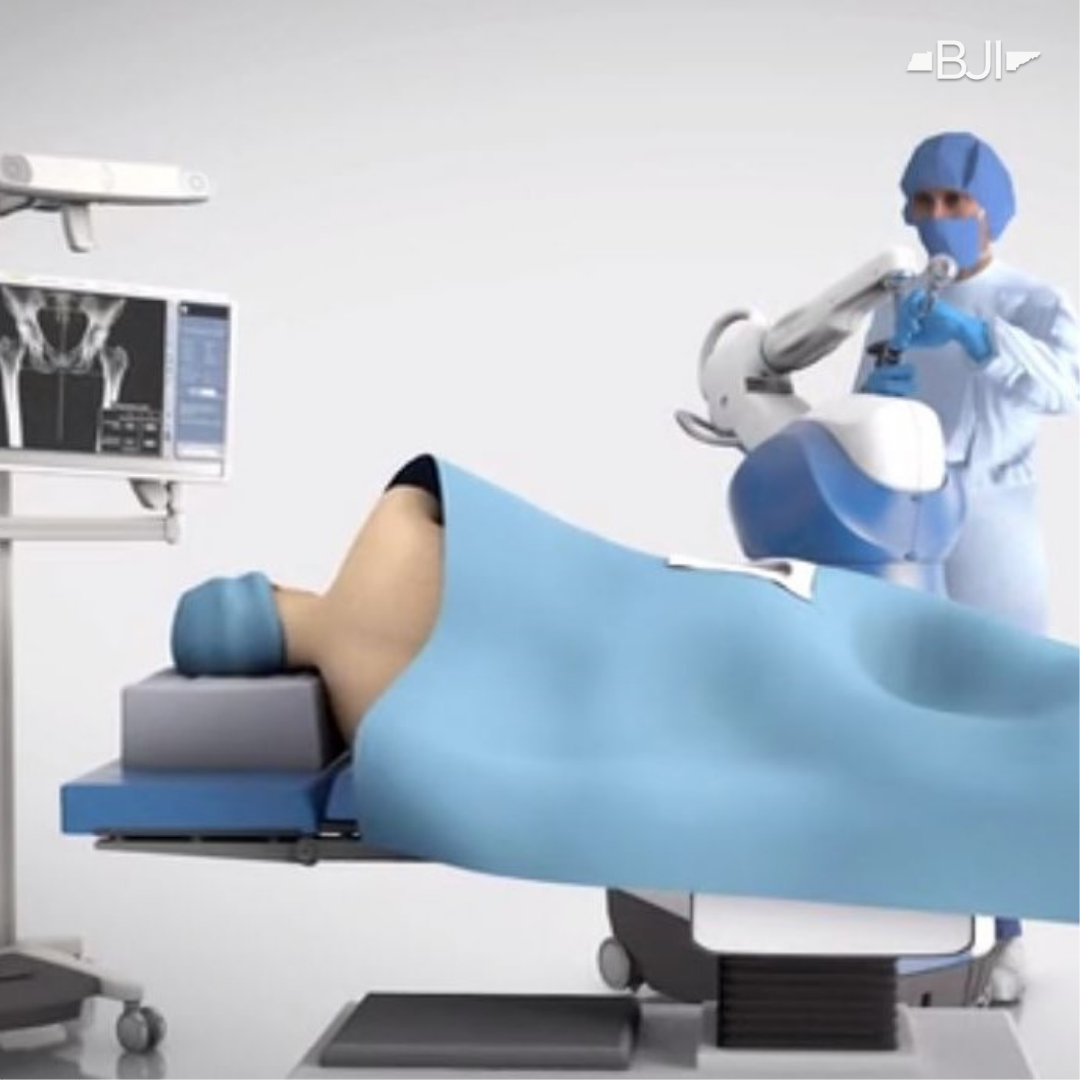
3D Modeling
Increasingly 3D modeling is used to provide surgeons with a precise 3D image of bone and joint structures. 3D modeling is accomplished with sophisticated computer programs and based on actual patient imaging (xray, CT, and/or MRI). As an example, we often use computer-generated 3D modeling (based on CT scans) to complete preoperative planning for knee and hip replacement surgeries.